Cancerous skin growths fall into three basic categories:
- Basal cell carcinomas (BCC) are the most common and most treatable. They present as a bleeding pimple like lesion that doesn’t heal, sores, scaly plaques of reddened skin, shiny, pink bumps, or a scar without cause. BCCs are usually caused by cumulative UV exposure, so they are classically seen on scalp, face, ears, neck, shoulders, and back. A BCC can become disfiguring but is rarely life threatening and doesn’t normally spread to other body parts.
- A squamous cell carcinoma (SCC) may appear as a red, scaly plaque, an open sore, or look like a wart. SCCs are also linked to UV exposure over a period of time. Skin injuries, autoimmune diseases, and some medications can trigger their development. Adults over the age of 50 and those who have had a BCC are more susceptible. With early detection and removal, SCCs are usually curable. However, this type of cancer results in about 2,500 deaths each year in the U.S. if allowed to metastasize to other organs.
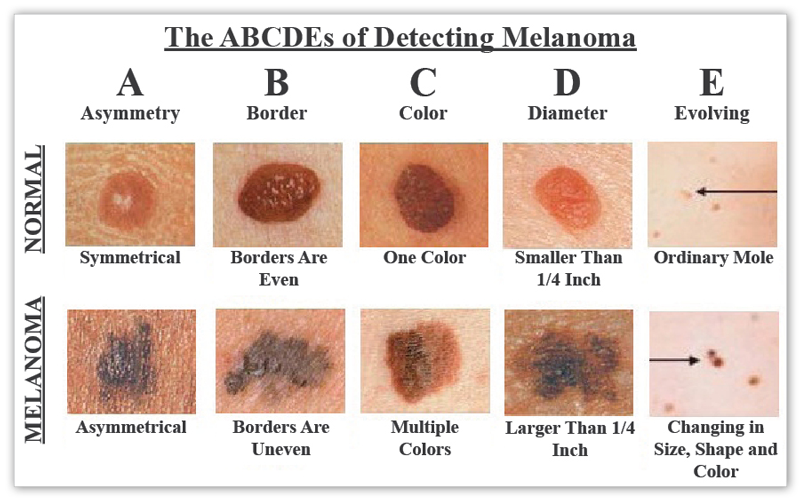
- Melanoma is the most formidable type of skin cancer. These malignant tumors often look like moles that are changing in size, color, or symptoms. While usually brown or black, they may be pink, red, purple, blue, white, or skin toned. Melanomas are triggered by intense UV exposure (sunburn) and likely have other environmental and genetic factors related to their development. Melanoma readily metastasizes, spreading to other organs. It kills nearly 9,000 Americans annually.
 The board certified dermatologists at Lupo Center for Aesthetic and General Dermatology first confirm diagnosis of a suspected skin cancer with a clinical biopsy. Treatment, usually on an outpatient basis, depends on the diagnosis but treatment options include surgical excision, electrocautery, topical prescription medications or our doctors may formulate a combination approach to eradicate the cancer. Depending on the location and size of the tumor and the patient’s health, they may recommend seeing a specialist for Mohs micrographic surgery – a more precise method that spares surrounding tissues. In some cases, traditional radiation or chemotherapy is indicated, and reconstructive surgery may be necessary.
The board certified dermatologists at Lupo Center for Aesthetic and General Dermatology first confirm diagnosis of a suspected skin cancer with a clinical biopsy. Treatment, usually on an outpatient basis, depends on the diagnosis but treatment options include surgical excision, electrocautery, topical prescription medications or our doctors may formulate a combination approach to eradicate the cancer. Depending on the location and size of the tumor and the patient’s health, they may recommend seeing a specialist for Mohs micrographic surgery – a more precise method that spares surrounding tissues. In some cases, traditional radiation or chemotherapy is indicated, and reconstructive surgery may be necessary.Don’t take chances with your skin or your health – schedule an annual skin cancer screening at the Lupo Center for Aesthetic and General Dermatology.





